Tetralogy of Fallot?
Tetralogy of Fallot is a congenital heart defect . It has four characteristics:
- Ventricular septal defect (VSD): a hole between the two bottom chambers (the ventricles) of the heart that eject blood to the body and lungs.
- Overriding aorta: the aorta, the large artery that takes blood to the body, is on top of both ventricles, instead of just the left ventricle as in a normal heart .
- Pulmonary stenosis : a narrowing of the pulmonary valve, the area below the valve, or the pulmonary arteries, which carry blood from the heart to the lungs.
- Hypertrophy: the right ventricle becomes thicker and more muscular than normal as a result of working harder to pump blood through the narrow pulmonary valve.
Listen to experts from the Cardiac Center explain the structure of a heart with TOF.
Signs and Symptoms
The symptoms of tetralogy of Fallot include:
- Blue or purple tint to lips, skin and nails (cyanosis)
- Heart murmur: the heart sounds abnormal when a doctor listens with a stethoscope
- In older children, abnormal shape of the fingertips (“clubbing”)
- Spells during which oxygen levels drop: lips and skin will become bluer, and the child will become fussy or irritable and then sleepy or unresponsive
Testing and Diagnosis
Tetralogy of Fallot may be diagnosed with fetal echocardiogram (ultrasound) before your baby is born. Our Fetal Heart Program will then prepare a plan for delivery and care immediately after birth.
Doctors might also make the TOF diagnosis before your newborn leaves the hospital if they hear a murmur or see a blue tint to the skin. Your primary care pediatrician might detect the same symptoms during a checkup. And sometimes a parent might notice TOF symptoms and bring the baby to a doctor or hospital.
Diagnosis of TOF may require some or all of these tests:
- Pulse oximetry: a painless way to monitor the oxygen content of the blood
- Electrocardiogram (ECG): a record of the electrical activity of the heart
- Echocardiogram (also called “echo” or ultrasound): sound waves create an image of the heart
- Chest X-ray
- Cardiac MRI : a three-dimensional image that shows the heart’s abnormalities
- Cardiac catheterization : a thin tube (catheter) is inserted into the heart through a large vein in the leg
A number of children with TOF also have genetic syndromes such as DiGeorge syndrome, Trisomy 21 (Down syndrome), Alagille syndrome or 22q11 deletion syndrome. Genetic testing (a blood test) may be part of an evaluation.
Treatment
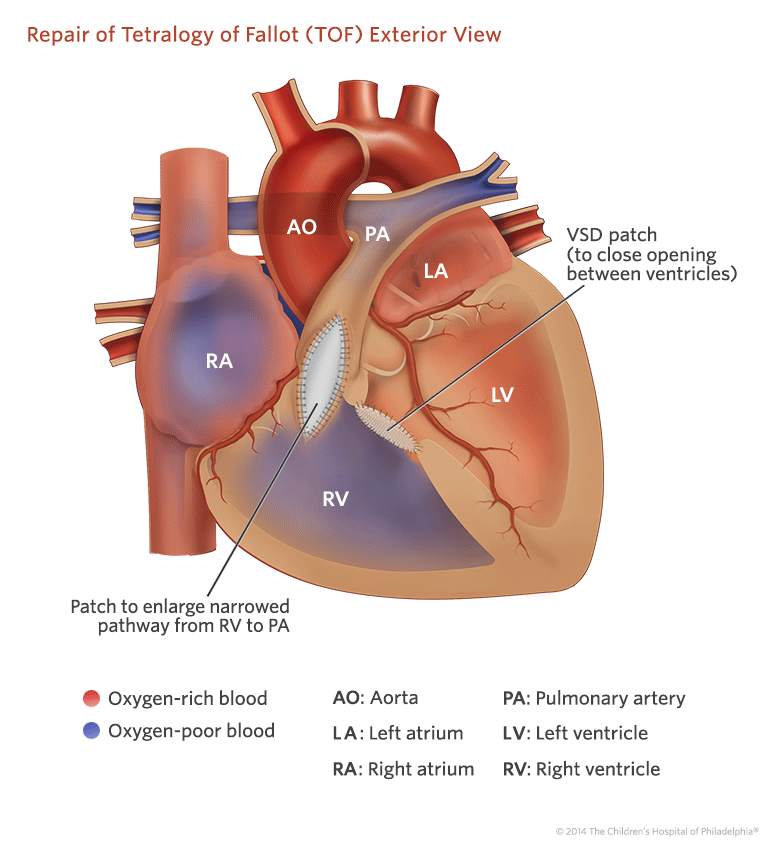
Surgery is required to repair tetralogy of Fallot. Typically in the first few months of life we will perform open heart surgery to patch the hole (VSD) and widen the pulmonary valve or artery.
In some cases, depending on the unique needs of the patient, we will perform a temporary repair until a complete repair can be done. The temporary repair involves connecting the pulmonary arteries (which carry blood from heart to lungs) with one of the large arteries that carry blood away from the heart to the body. This increases the amount of blood that reaches the lungs, and so increases the amount of oxygen in the blood.
After surgery, your child will initially recover in the Evelyn and Daniel M. Tabas Cardiac Intensive Care Unit (CICU) and then in the Cardiac Care Unit as she improves.
Outlook
Because of enormous strides in medicine and technology, today most children born with heart conditions like tetralogy of Fallot go on to lead healthy, productive lives as adults.
Sometimes children with TOF experience heart problems later in life, including a leaky heart valve and irregular heartbeat (arrhythmia). Medicine or repeat surgery may be required.
Follow-Up Care
Through age 18
If your child has had surgical repair of tetralogy of Fallot, she will require lifelong care by a cardiologist.
Our pediatric cardiologists follow patients until they are young adults, coordinating care with the primary care physician. Patients will need to carefully follow their doctors’ advice, including staying on any medications prescribed and, in some cases, limiting exercise.
Into adulthood
We will help patients transition care to an adult cardiologist. The Philadelphia Adult Congenital Heart Center , a joint program of The Children’s Hospital of Philadelphia and Penn Medicine, meets the unique needs of adults who were born with heart defects like TOF.

